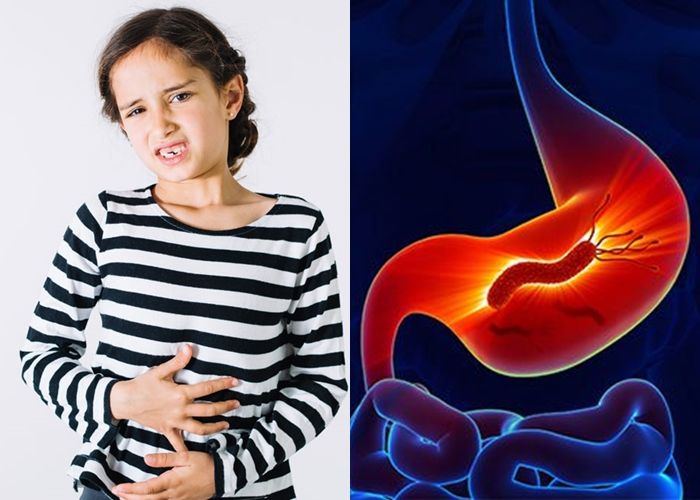
Helicobacter pylori is one of the bacteria playing an important role in a variety of spectrum of gastrointestinal diseases, ranging from gastritis – or commonly known as ulcer – to malignant gastric cancer. In the population of children themselves, Helicobacter pylori can cause bad breath, stomach ulcers, recurring vomit, iron malabsorption, and chronic gastritis.
Previous reports have stated that about a third of children worldwide have been infected by Helicobacter pylori, without showing significant symptoms. However, in Indonesia, it was found that only about 3.8% of children were infected by Helicobacter pylori. It makes us think, whether the diagnostic methods used so far, in Indonesia have been sensitive enough to detect the presence of Helicobacter pylori infection.
Based on European (ESPGHAN) and North American (NASPGHAN) guidelines, the standard diagnostic method for detecting Helicobacter pylori infection is the endoscopy-biopsy method. Unfortunately, this method is very invasive, high risk, expensive, uncomfortable for the patient, and must be done by trained medical personnel.
Another recommended method is to use the urea-breath test. Although it is quite sensitive and specific enough to diagnose Helicobacter pylori infection, this method is also quite expensive and involves radioisotopes. Therefore, in our study, we wanted to compare the sensitivity and specificity of other methods including the stool antigen method using faecal samples, the ELISA method using salivary immunoglobulin, and the ELISA method using blood samples (serum immunoglobulin) to the endoscopy-biopsy method.
In this study, we involved 37 children who came to Dr. Soetomo General Hospital, Surabaya, from May to July 2012 suspected with Helicobacter pylori infection. The patients included in this study were patients aged 3-18 years, showing symptoms of Helicobacter pylori infection such as experiencing at least 3 episodes of abdominal pain in the last 3 months, and showing symptoms of dyspepsia, such as recurrent epigastric pain, discomfort in the stomach, bloating, nausea, vomiting, full satiety, and abdominal distension in the last 3 months.
Our research results showed that ELISA method with saliva is sensitive and specific enough to confirm Helicobacter pylori infection, compared to the endoscopy-biopsy method and the urea-breath test. This method is much simpler and more convenient for patients because it only uses their saliva for the laboratory tests.
The patient’s saliva can be collected in a tube, then tested in a laboratory to see the presence of antibodies in the saliva. Compared to ELISA method using blood samples, this method does not increase the risk of infection in patients because it does not require blood collection with a syringe. The test cost is also far cheaper than the endoscopy-biopsy method.
A similar study in the UK also showed that ELISA examination using saliva was sensitive and specific enough to detect Helicobacter pylori infection. However, this method also has some disadvantages. In this method, antibody values can be detected high if the patient also has periodontal abnormalities or gum bleeding so in patients with dental and oral abnormalities can be over diagnosed.
On the other hand, when the value of antibodies in saliva is lower than the bottom threshold which can be diagnosed by ELISA test, the patient may occur under diagnosis. Moreover, this method cannot be used to evaluate therapeutic results because the antibodies in the saliva can remain high for a long time, even if the patient has no symptoms.
Thus, we concluded that the ELISA method using saliva can be used as a diagnostic method for Helicobacter pylori infection in children. Other methods we tested in this study, such as the stool antigen method using fecal samples and the ELISA method using blood samples, can be used as an alternative non-invasive screening test for Helicobacter pylori infection. However, both methods still cannot be used as diagnostic methods because although the stool antigen method and the ELISA method with blood samples have high sensitivity, their specificity is low.
Author: Andy Darma
Details of the research available at