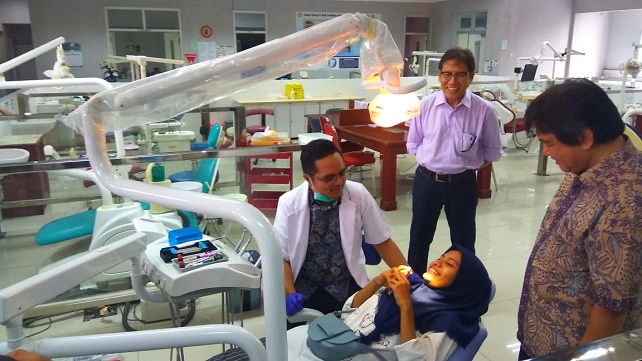
Infection is a serious health problem faced by many countrie (Khanghahi et al,2013). Dental technicians are one of the occupations that are at risk of contracting an infectious disease that can occur from transmission through saliva, blood, or contaminated equipment. Dental impression sent to the dental laboratory always contain saliva and sometimes blood. These saliva and blood can contain many non-pathogenic and pathogenic microorganisms such as Candida albicans, Streptococcus aureus, viral Hepatitis, herpes simplex, HIV and others. Dental laboratories are areas where dental technicians can get infected especially when conditions are unsterilized. It is difficult to disinfect the mold because microorganisms can enter the inside part of the cast so as to make disinfection less optimal. Bacteria in the oral cavity can stay alive for a week even within gypsum. Therefore, all dental impression received from the dentist must be disinfected.
Technicians working in the dental laboratory can be exposed to infection through direct contact with items that have not been disinfected through cuts and abrasions while working without using gloves and masks. Infection can be transferred through dental impression performed by dental technicians related to surface contact, hand pieces, burs, pumice, aerosols, etc. Dental laboratories must be as safe as possible from any type of infection. The potential for disease transmission can be minimized through;
(a) Immunization, especially hepatitis B.
(b) Barrier
Techniques include hand washing with antimicrobial soap or rubbing hands with alcohol-based ingredients before starting work in a dental laboratory. When working, a dental technician must always use personal protective equipment such as gloves, masks, glasses, and laboratory coats. Gloves must be used when cleaning or filling dental impression. Mask, protector glasses or clothing must be used when there is potential for splashing, spraying, or aerosols such as when operating a machine while polishing, cutting the casting results, etc.
Laboratory coats must be used at any time during the fabrication process in the laboratory and replaced or washed every day and may not be used outside the laboratory. This prevents transmission from the laboratory towards environment or vice versa. All disinfection procedures must be carried out in a laboratory by trained technicians if the disinfection status is unknown. Disinfection must be correct to prevent corrosion of metal components, dimensional changes and surface texture of the work. Some effectiveness of disinfectants has been reported, including chlorhexidine digluconate and glutaraldehyde. Infection control is considered to be a very important concern in the dental laboratory so that dental technicians can avoid cross infection. This study aims to determine the implementation of disinfection in dental laboratories in East Java as a preventive measure and control of cross infection.
Efforts to prevent and control cross infection in the dental laboratory need to be done considering that the dental laboratory can be a source of transmission of infectious diseases originating from oral pathogens and respiratory tract microorganisms. Pathogenic microorganisms such as hepatitis B virus, hepatitis C virus, HIV / AIDS, herpes simplex virus, cytomegalovirus
(CMV), Mycobacterium tuberculosis, staphylococci, streptococci and other viruses and bacteria. The dental laboratory accepts the work of fabricating fixed tooth restorations, partial or full dentures, removable orthodontic appliances, or its reparation from the clinic. Clinicians can send their orders to the dental laboratory in the form of dental impression, dental models or removable denture prostheses as well as plates of removable orthodontic devices that require reparation. If the material has not been disinfected by the clinician, it may contain pathogenic microorganisms that can cause crossinfection in the dental technician who is working on it, as well as dentists and other patients. Dentists as personnel who provide health services should conduct infection prevention and control.
Respondents in this study were dental laboratories located in the area of East Java Province which had been operating at least 1 – 5 years (20%), 16 – 20 years (35%) and more than 20 years (25%). This shows that respondents have had enough time or experience to carry out their functions. During dental laboratory operational, it turned out that 90% of respondents did not disinfect the workspace, equipment or materials received from the dental clinic and only 10% did it. Of the 10% who disinfected there was only 1 respondent who did it every day. This result is similar to the results of a survey of infection control practices in a private dental laboratory in Riyadh and found that 87.5% of respondents were unaware and did not follow infection control procedures.
Prevention and control of cross infection procedure in dental laboratories in East Java Province is still low. Guidance and supervision of the operation of the dental laboratory by the Indonesian government and professional organizations needs to be improved. Education regarding infection control needs to be done through trainings and incorporating material on infection control in the dental technician study program curriculum in Indonesia.
Author: Eny Inayati drg,.M.Kes
Detailed information from this study can be seen on our article at:
https://e-journal.unair.ac.id/JVHS/article/view/26180/13811
Eny Inayati, Sri Redjeki, Nanda Rachmad Putra Gofur. PREVENTION AND CONTROL OF CROSS INFECTION AT DENTAL LABORATORIES IN EAST JAVA PROVINCE OF INDONESIA. Journal of Vocational Health Studies 04 (2021): 125-130