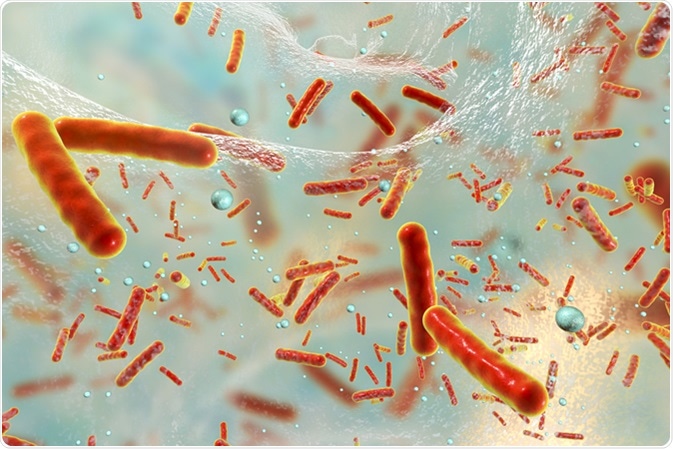
In the human oral cavity, there are various kinds of microorganisms, both in the form of normal flora and pathogens. Oral bacteria develop with the composition and structure of complex species to maintain their attachment to a surface. Each bacterium can defend itself for survival, such as exposure to chemicals, physical pressure, and radiation. One form of bacterial defence is the formation of biofilms.
A biofilm is a collection of microorganism cells, especially bacteria, which are attached to a biological or inanimate surface and are covered by a carbohydrate adhesive produced by bacteria. Biofilms are nutrient traps for the growth of microorganism populations and help prevent the release of cells from the surface of living or dead objects. The surface where the biofilm is attached is an important habitat for microorganisms because nutrients can be trapped on the surface so that the nutritional content can be higher than in liquids.
The formation of biofilms is caused by several things; first the bacteria defend themselves from phagocytosis of host immune system cells and the penetration of toxic molecules such as antibiotics. Second, the formation of biofilms allows cells to remain in favourable locations, such as attaching to nutrient-rich surfaces, such as tooth surfaces that can supply food to bacteria continuously. Third, biofilms are formed to be closely interconnected between bacteria with each other so that it can increase the chance of survival. Besides, when cells are close to one another, there is more opportunity for nutritional and genetic exchange, besides that biofilms are also a natural way of life for some bacteria due to limited nutrition so they can live in symbiosis, unlike rich artificial media for nutrition for bacteria.
Biofilms consist of microbial cells and extracellular polymeric substance (EPS). EPS can cover 50% to 90% of the total organic carbon biofilm and can be considered a primary matrix biofilm material. In line with its growth, these biofilm cells will produce Extracellular Polymeric Substances (EPS), which will attach bacteria to the surface and attach to form a microcolony. If the cells continue to grow and form a thicker layer, the microbes attached to the innermost layer of the surface will lack nutrients – and accumulate toxic bacterial products. The easiest example of biofilm is biofilm in the oral cavity called plaque.
Streptococcus mutans (S. mutans) is a bacterium that is generally found in the oral cavity and includes normal flora. These bacteria produce products in the form of lactic acid and are the main bacteria for the formation of plaque on the surface of the teeth and carry out fermentation of diets that contain lots of carbohydrates and proteins. The results in the formation and accumulation of acids, which declassification and destruction of dental tissue under the plaque and this condition are found in the process of formation of dental caries.
Streptococcus mutans is a gram-positive bacteria, is facultatively anaerobic, in the form of coccus (round) and arranged like a chain. Aggregatibacter actinomycetemcomitans (A.a) is also included in the category of the normal flora of the oral cavity can colonise the mucosa of the oral cavity, teeth and oropharynx and can change properties to be opportunistic pathogens. These bacteria can form biofilms as an effort to cope with changes in the environment. This bacterium also plays an important role in the formation of subgingival plaque that causes periodontitis. Aggregatibacter actinomycetemcomitans is one of the gram-negative bacteria that is facultatively anaerobic. Streptococcus mutans and Aggregatibacter actinomycetemcomitans are bacteria that can form biofilms and produce Extracellular Polymeric Substances (EPS).
Sucrose is a type of carbohydrate that can help the formation of biofilms and bacteria attachment to the tooth surface. Some proteins have been shown to function as high-affinity adhesins and play a central role in the initiation of biofilm formation. Recent genomic and proteomic studies have identified many gene expressions, and differential gene products declared to be influential during biofilm formation. This gene has been identified to encode polypeptides expressed in a phenotype form. A recent example has identified a gene that is brpA (for regulatory protein biofilms), the loss of brpA in Streptococcus mutans causes failure in biofilm formation on abiotic surfaces. Whereas in Aggregatibacter actinomyctemcomitans identified that the RbsB and LsrB genes influence the growth of the wild-type biofilm. Thus, special treatment of gene removal on biofilms is thought to reduce bacterial virulence.
Author: Indah Listiana Kriswandini
Detail information about this article can be seen in our article at:
https://www.ncbi.nlm.nih.gov/pubmed/31169162
Indah Listiana Kriswandini, Markus Budi Rahardjo, Hendrik Setia Budi, Risma Amalia. 2019. The difference in biofilm molecular weight in Streptococcus mutans and Aggregatibacter actinomycetemcomitans induced by sucrose and soy protein (glycine soja). Indian J Dent Res. 2019 Mar-Apr;30(2):273-276. doi: 10.4103/ijdr.IJDR_183_17.